Proton therapy is an external beam radiation therapy that uses protons, which have unique properties allowing the precise targeting of tumor cells. Unlike photons, used in traditional radiation therapy, protons have a Bragg effect, which delivers the bulk of the energy into tumor cells and prevents damage to healthy tissue.
Protons versus Photons
Proton beam therapy differs from conventional radiation therapy by using positively charged high-energy proton particles to target cancer cells with extreme precision. A cyclotron accelerates protons to very high speeds sending them directly into the tumor. There, the positively charged protons interact with negatively charged electrons in the cancer cells, causing damage to the cells' DNA, killing them.
Proton beam therapy is unique in that you can adjust the beam so that it deposits its maximum energy at the tumor site. This Bragg effect, not possible with photon beam radiation, spares healthy tissue beyond the tumor.
Photon beam radiation is the most common type of radiation therapy, and, like X-rays, it emits radiation throughout its entire tract. Because photon beam radiation doesn't exhibit a Bragg effect, its delivery to the tumor is not as exact as proton beam therapy.
Prior photon beam therapy
Four weeks after my prostatectomy, starting in August of 2022, I underwent intensity-modulated radiation therapy (IMRT) to my pelvis. IMRT is a photon-based radiation that uses linear accelerators to deliver precise doses of radiation, but not as precisely as proton-based radiation therapy.
Optimally, you want to be able to image a tumor before you treat it with IMRT so that you can focus the radiation on the cancer. When I underwent IMRT, my positron emission tomography (PET) computerized tomography (CT) scan did not show cancer. So, my radiation oncologist focused the radiation where he thought the tumor would likely be - the prostate bed and pelvic lymph nodes.
When I had the prostatectomy, the surgeon removed nine lymph nodes from my pelvis, two of which contained cancer cells. The tissue from the surgery also showed positive margins, meaning the tumor cells extended to the edge of the tissue removed. Positive margins indicate some cancerous tissue was likely left behind. So it made sense to focus on the lymph nodes and where the prostate used to be.
If my prostatectomy had surgically cured the prostate cancer, my prostate-specific antigen (PSA) level should have been zero, but it was 4.9. The lowest my PSA got after IMRT was 0.9, and it has steadily risen since then. Prior to starting proton beam therapy, my PSA tumor marker on December 15, 2022, was 57.64.
Current proton beam therapy
My most recent prostate-specific membrane antigen (PSMA) PET CT scan on December 15, 2022, showed six tumor areas in the lymph node chains in my abdomen on each side of my aorta. We decided to "paint" the lymph node chains on each side of my aorta and "boost" the proton energy in the areas lighting up on the PET scan.
The theory behind this approach is to focus high levels of proton beam energy on the metastatic tumor sites and to treat the entire lymphatic chain, which most likely contains micrometastases not visible on the PET scan.
Planning for proton therapy
The PET CT scan captures detailed images of the tumor and surrounding structures, which lets the medical team precisely locate the tumors and their proximity to my organs.
The top two lymph nodes were in the retrocrural space near my heart and stomach. The lymph node near my left common iliac artery was in an area previously treated with radiation putting me at a higher risk for complications. Despite these issues, my radiation oncologist felt he could safely treat these areas due to the preciseness of proton beam therapy.
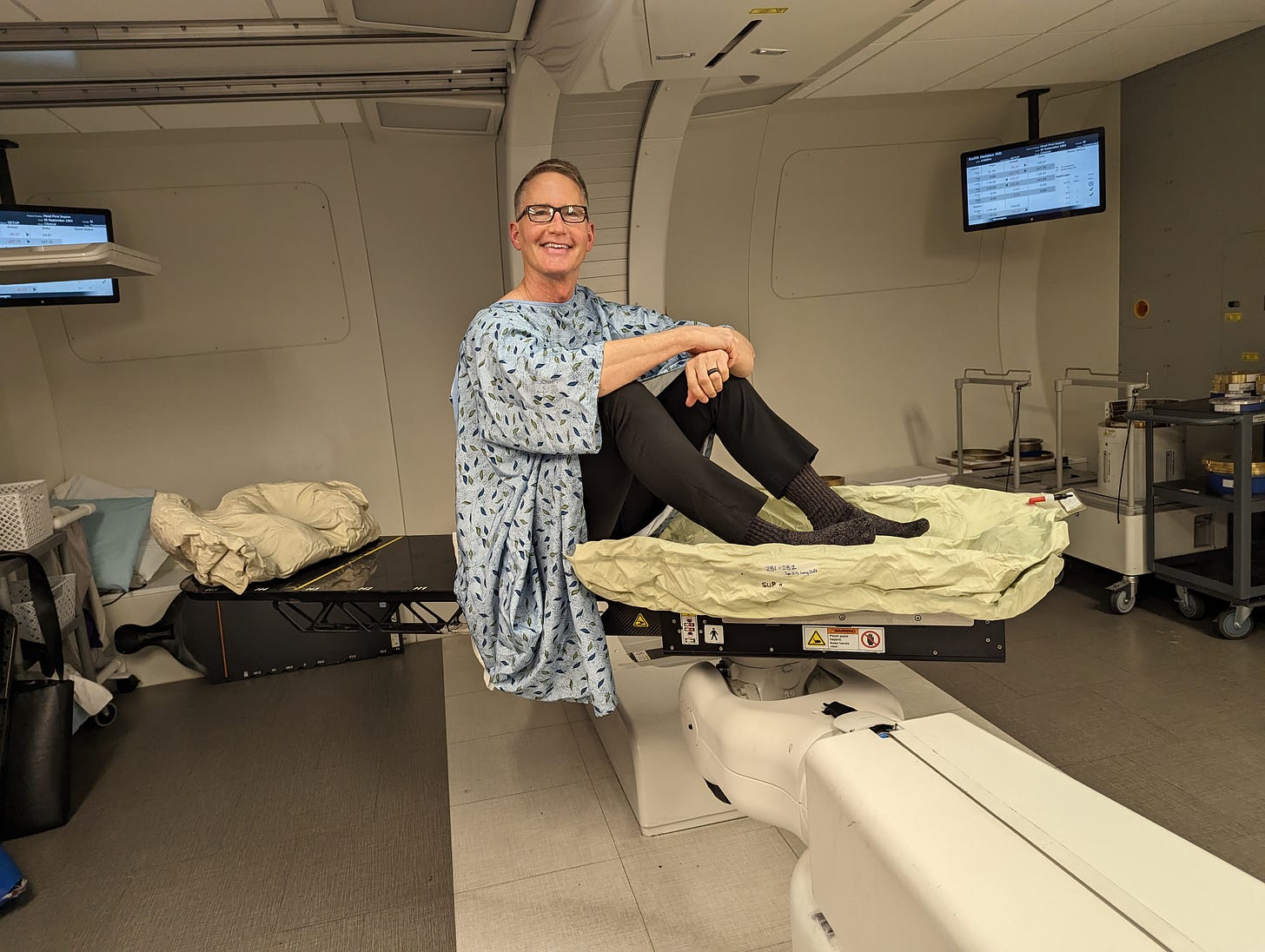
I underwent a "planning" CT scan where I laid on a table in the same position I would be in during treatment. The technicians created a mold from material similar to a bean bag and pumped air into the mold to hold me in a consistent position. Each time I underwent proton therapy, I lay in this mold with my arms held above my head.
During the planning CT, the technicians used a Sharpie pen to mark my skin to help align me with the machine. Then they covered the marked areas with clear round adhesives so the marks wouldn't disappear when I showered. During treatment, I lay on a computer-controlled table, which the technicians moved to align the spots on my skin with lasers in the proton room. This alignment helped accurately direct the proton beam.
The planning team, including my radiation oncologists and a medical physicist, analyzed the CT images with special software to delineate the tumor and nearby healthy structures. This treatment planning software helps define the target volume. It determines the optimal beam angles, proton energies, and other parameters to deliver the prescribed dose to the tumor while minimizing radiation to healthy tissues.
Go Time
My first day of proton therapy on January 10, 2023, was a simulation where the medical team simulated my treatment without applying the proton beam energy. We did a run-through to ensure the table would move adequately and everything would line up as planned.
The next day, we began the proton beam treatment five days a week for seven weeks. I drove to the radiation center every day after work and lay on the treatment table for about twenty-five minutes while the proton beam did its thing.
I got used to the movements of the machine and table lining me up correctly for the proton beam. In between these movements, the technicians would move an X-ray machine over my thorax to help ensure the correct alignment of my body. I could barely see the technicians through a protective wall with a thick plate of glass, making sure the X-ray indicated adequate positioning of my body.
Sometimes, the technician would have me move toward the side of the table or tug on the sheet underneath me to rotate my body slightly. Intermittently, the red laser lights would come on, and the technicians would check to make sure the laser lights aligned with the marks on my skin.
The technicians would also intermittently change the solid metal tips at the nozzle where the proton beam left the machine before entering my body. Specially made for my treatment, these metal tips direct the proton beam to ensure energy enters the tumor and avoids healthy tissue.
Just before each time the proton machine turned on, the technicians would scurry out of the room to safety. I'd hear the machine kick on with a low-pitched rumble, and I began my visualization of the protons shooting all of the cancer cells into oblivion.
The device would power down, and I'd hear their voices getting louder as they came back down the hall into the room. Then they'd start again with the nozzle tip changes and bed and machine movements for the next angle of attack.
People you meet along the way
Each day I arrived at the radiation center, I'd check in and go directly to put on a medical gown. Then I'd sit in the proton treatment waiting room, separate from the regular one. It is beautiful, modern and has an area by the window where you can make coffee or tea and get snacks like an apple.
The proton machine is booked out far ahead of time from early morning until about nine o'clock at night. My start time was 3:10 pm, but it didn't always happen on time. Some days the machine would need a battery change or repair work and delay things, but that didn't happen often.
You got used to seeing and getting to know mostly the same patients before and after you on the schedule, but occasionally that changed as some patients finished their treatment and others started theirs. Almost everyone knew what type of cancer the other patients had, either from hearing it directly from them or hearing them tell another patient their story.
We were like a club, rooting for each other and wishing each other a good day as they left. There was one guy I resonated with more than everyone else. He looked younger than me and had survived lung cancer for almost ten years. He, too, had received prior radiation therapy, and this was his first proton therapy.
He and I chatted the most, and I grew to like him as a fraternity brother. I looked forward to speaking with him each day I'd go for therapy. His treatment ended before mine, and on his last day, we shook hands. I looked him straight in the eye, and with a big smile, I said, "I hope I never see you here again." He smiled back and said, "I wish the same for you." Sometimes I think about him, and hope is doing well.
Earth angels
It's hard to describe how the proton technicians made me feel welcome and comfortable. I felt safe in their hands and trusted they knew what they were doing with this incredibly powerful machine.
They all were very friendly and greeted me each time like I was a loved family member. Despite our relatively short time together, we learned a little about each other. They profusely thanked me when I brought them the chocolate cake that my sister had made.
When each treatment ended, they would cheerfully tell me to have a good rest of my day, and I'd wish them the same. One of them usually asked if I wanted my hospital gown tied before I returned to the dressing room. And I always took them up on the offer because it was challenging for me to do with the ties behind the gown.
Side effects of proton therapy
I purposely didn't read up about the side effects of proton therapy because I didn't want to induce the nocebo effect. I had previously read that it caused fatigue, so I was anticipating that, but I had no idea how tired it would make me.
About one week into treatment, I started waking up very tired in the morning and would get exhausted by the end of the work day. Despite taking Mondays off work during proton therapy, the exhaustion progressed the longer I underwent treatment.
I started taking a one to two-hour nap when I got home from treatment, waking up to eat dinner, going for a walk, showering, and going to bed by nine pm. On weekends, I'd sleep ten to twelve hours each night. Sleep was becoming my best friend.
Thankfully, I had enough energy to go to the gym on the weekends and walk most weekday evenings. As I write this, my energy level has yet to return to my baseline four months after proton therapy. It probably didn't help that I had Covid the week before starting proton therapy despite being vaccinated and boosted.
Another strange side effect I had was that I began to crave meat. I usually eat vegetarian during the week and have a small amount of animal protein and fish on the weekends. But during proton therapy, eating my mostly plant-based meals was difficult.
In addition, I began to experience intermittent low-grade nausea, a common side effect of proton therapy. I also began to have something rare for me, constipation. My doctor prescribed Zofran for nausea, which made the constipation worse. A switch from Zofran to Compazine controlled my nausea and improved my constipation.
I experienced one more side effect, and that it's what I call my proton sunburn. I called it a sunburn because it eventually turned brown like a tan. It never blistered, and it wasn't painful. It just itched a bit after a shower.
The ending
Ending proton therapy was bittersweet. I enjoyed my visits with the very outgoing and friendly proton technicians. I also felt a sense of safety knowing I was doing something very proactive five days a week to eliminate this cancer. In the five years since my last radiation therapy, I have been fighting it independently with lifestyle and nutritional approaches as I watched my PSA tumor marker slowly rise.
On my last day of proton therapy, February 24, 2023, I brought the technicians roses, thanked each one of them, took pictures, and gave them each a hug. I am genuinely thankful for their work, especially how they do it - with compassion and kindness.
My radiation oncologist recommended we wait three months after proton therapy until my next PSA level and PSMA PET CT scan. You'd think I'd be used to the waits, but I'm not. You go on with your life, hoping for the best outcome, and surrender to trust.
I plan to start sending out this newsletter every two weeks from this point forward. Not that more things are happening to me, but I want to make this newsletter more educational, which requires more frequent writing.
In the following newsletter, I'll tell you the outcome of my post-proton PSA and PET CT scan. The results may surprise you. They did me. Until then, lots of love and peace to everyone.
Keith R. Holden, M.D.






Big love to you Keith, thank you for generously sharing your journey. What a love are you! 💛💚💜